Turn Tough Veins Into Confident Skills
Difficult venipuncture is one of those real clinical moments that can turn a calm shift into a stressful one. A nurse needs labs on a dehydrated or elderly patient, everyone is busy, and the veins just are not showing up. If you are a CNA or preparing for phlebotomy training, this can feel scary fast.
Hard sticks are common in real-life care. We see them with Georgia’s aging population, patients with chronic illness, people who are dehydrated from allergies or from being outside in warmer weather, and those in hospitals or long-term care. In this guide, we share a simple playbook you can carry into your next shift, so you know how to spot a challenging vein, what safe adjustments the team can make, and when it is time to stop and call for help to keep the patient safe.
Reading the Vein Map Before You pick up a Needle
Before anyone even opens a needle, the first skill is learning to read the “vein map.” Good vein selection can turn a difficult draw into a smooth one.
In most cases, the priority list looks like this:
- First choice: Median cubital vein in the antecubital fossa
- Second choice: Cephalic vein
- Third choice: Basilic vein, and only if safer sites are not available
At the same time, there are areas that should be avoided:
- Sites with edema or swelling
- Arms with a dialysis fistula or graft
- Areas with redness, infection, or injury
- Spots close to a recent IV or previous stick that is still tender
Different patients bring different challenges. Elderly and long-term care patients often have fragile, thin, or “rolling” veins. Patients with obesity may have veins that are deeper and harder to feel. Anxious, confused, or pediatric patients may move right when the needle is going in.
Even before formal phlebotomy training, CNAs can help by sharpening assessment skills:
- Use unhurried visual inspection under good light
- Gently palpate with the fingertip, not poking or pressing too hard
- Compare both arms instead of locking in on the first vein you see
- Ask the patient where blood draws have worked well in the past
These steps shorten trial and error and show respect for the patient’s body and comfort.
Smart Positioning, Warming, and Hydration Checks
Body position can make veins easier to access. Small changes can bring a vein closer to the surface without causing strain for the patient.
Good positioning usually includes:
- Arm supported on a flat surface at or just below heart level
- Hand relaxed, not pumping a tight fist over and over
- The arm straight but not locked, with no twisting of the wrist
Pumping a fist too much can affect lab results and create more tension. A calm, supported arm gives better blood flow and less movement.
Warming the area is another simple tool the team can use. Warmth helps veins dilate and stand out, especially in cool exam rooms or early mornings. CNAs can often assist with:
- Applying a warm, moist towel or warm compress for 5 to 10 minutes
- Always checking the temperature inside the towel first to prevent burns
- Keeping the skin dry enough after warming so adhesive will stick properly
Hydration and circulation matter too. Dry mucous membranes, darker urine, confusion, or a recent stomach illness can all be clues that a patient is dried out. Gentle questions can help:
- “Have you had much to drink today?”
- “Have you been out in the heat a lot?”
When allowed and safe, encouraging appropriate oral fluids ahead of scheduled blood work can support better veins. Even when fluids cannot be given, just knowing the patient may be dehydrated helps the team plan for a tougher stick.
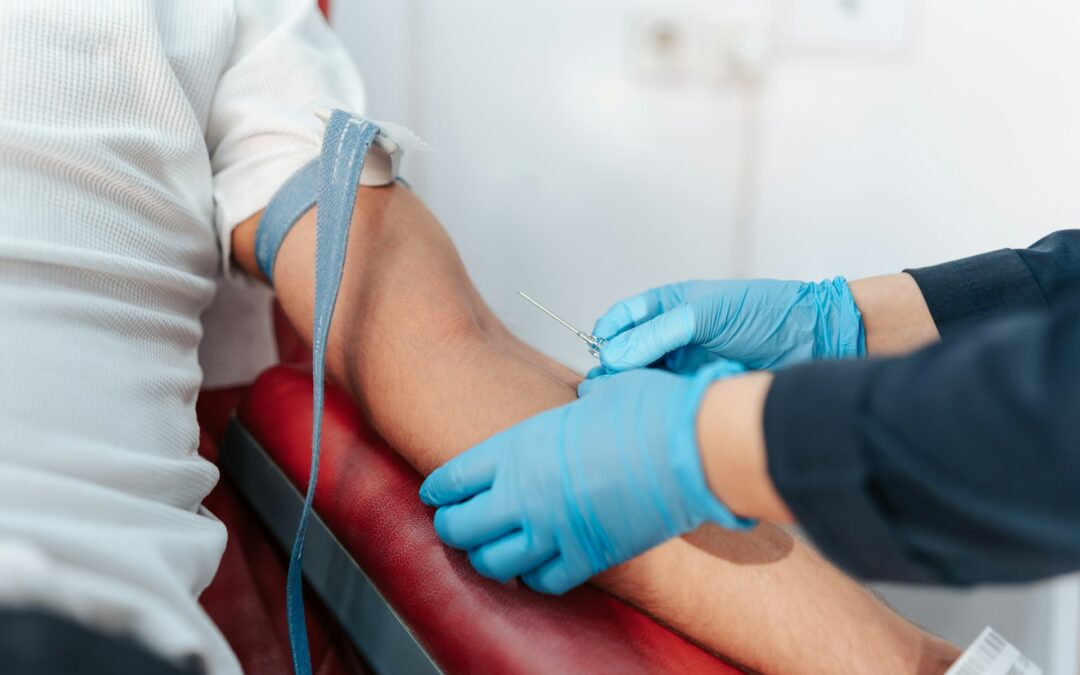
Technique Adjustments and Device Choices for Difficult Veins
Before a venipuncture is called a failed stick, trained staff can make small, careful adjustments. As a CNA, your role is to understand what safe technique looks like, support the licensed professional, and protect the patient.
Small, safe adjustments might include:
- Changing the needle angle slightly without digging
- Gently advancing or withdrawing a millimeter or two
- Firmly anchoring the vein below the puncture site to steady a rolling vein
What should never happen is “fishing” or sweeping the needle side to side inside the tissue. That kind of probing causes pain, bruising, and can damage the vein. If blood flow stops, the problem might be:
- Tube not fully seated
- Loss of vacuum in the tube
- Bevel resting against the vein wall
- Tourniquet left on too long, causing backflow issues
In those cases, the right move is to calmly check each factor, not to twist or jab the needle around. Knowing what not to do is as important as knowing the right steps.
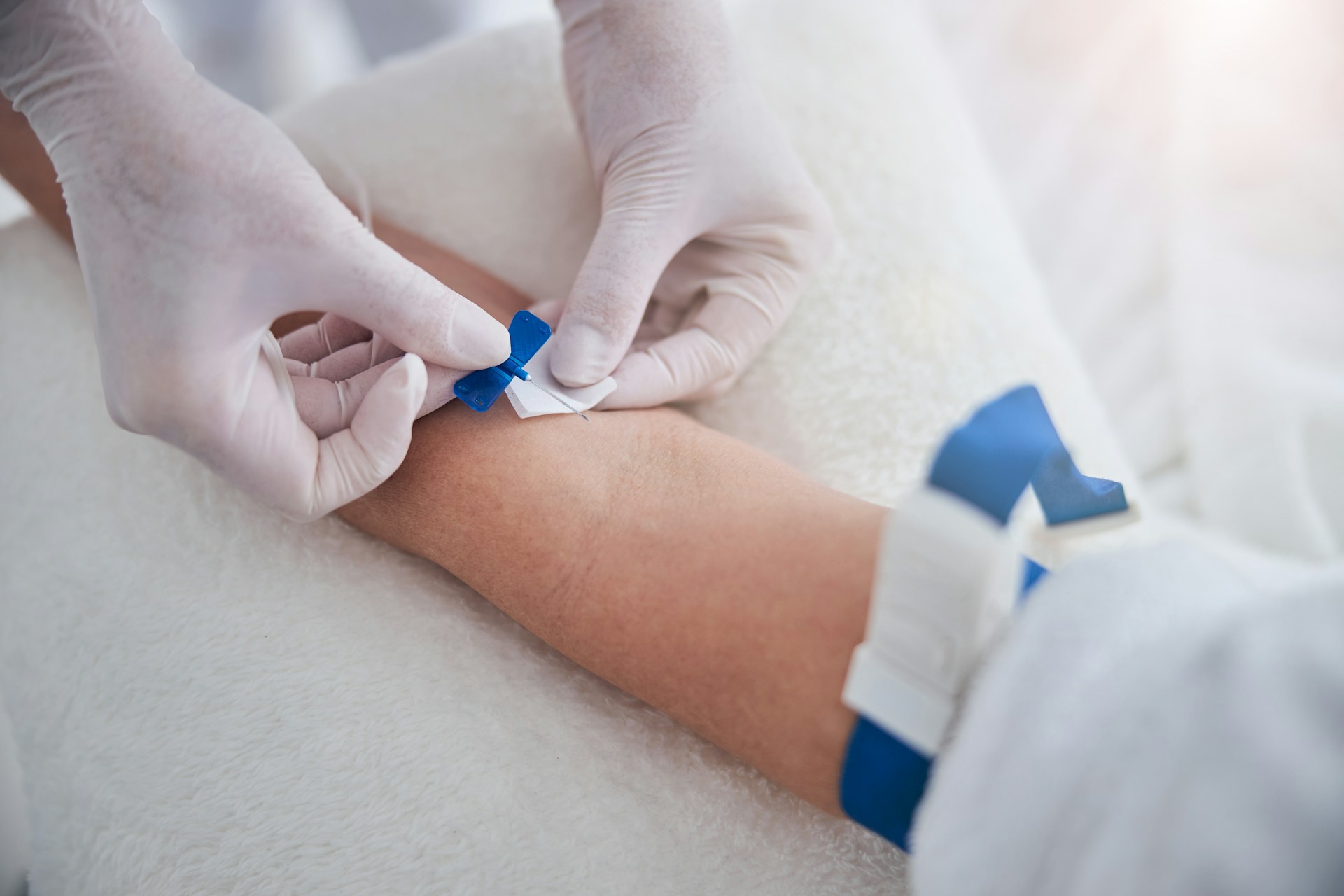
Device choice also plays a big part in success. For fragile or small veins, many teams prefer:
- Butterfly sets, which allow slower, more controlled entry
- A smaller gauge needle to reduce the chance of vein collapse
- Smaller-volume tubes so the vacuum pull is not as strong
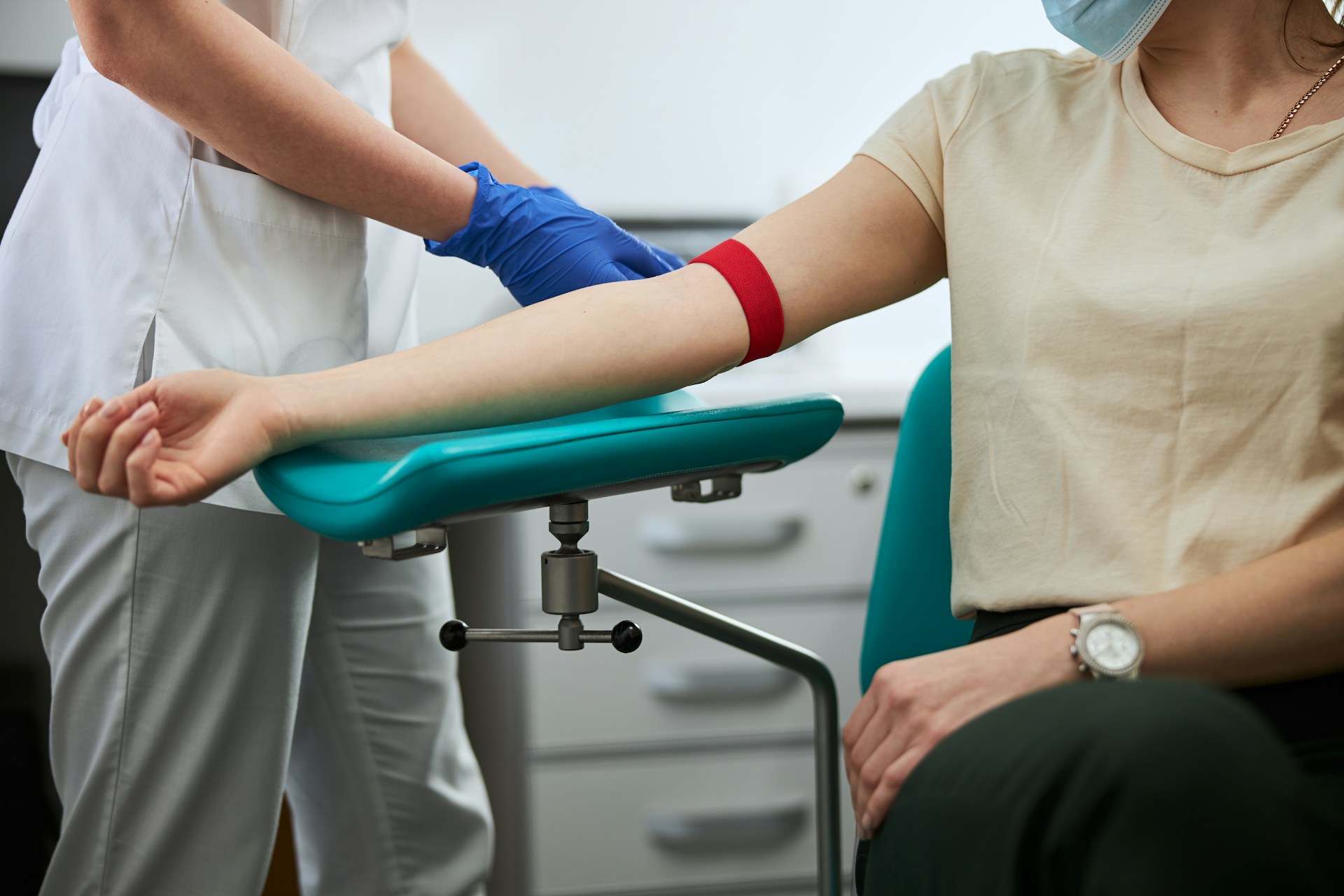
Healthier, larger veins can often handle straight needles and larger tubes for quicker draws. Tourniquet use also matters. Too tight or left on too long can cause pain, vein blowouts, or altered lab results. Good practice is to:
- Place it snug, not painful
- Release it as soon as blood flow is steady
- Never leave it on longer than needed for the draw
Hands-on phlebotomy training helps students feel the difference between these devices, learn their limits, and stay within Georgia guidelines and their facility’s policies about what tasks CNAs can and cannot do on their own.
When to Stop, Escalate, or Try Again Later
Knowing when to stop is a sign of skill, not weakness. Many facilities set clear limits, such as two attempts per person, before another team member must try. Repeated sticks raise the risk of:
- Hematomas and bruising
- Patient fear and loss of trust
- Delays in care and possible complaints
There are also moments when the attempt should stop right away, even on the first stick. Warning signs include:
- Sudden sharp, shooting, or electric pain that may signal nerve involvement
- Rapid swelling or a dark lump forming under the skin
- The patient becoming dizzy, pale, sweaty, or saying they feel like they might pass out
CNAs play a key part in spotting these reactions, speaking up, and supporting the patient. This might mean lowering the head of the bed, raising the feet if allowed, staying calm, and getting a nurse or phlebotomist quickly.
Escalation often means:
- Asking a more experienced phlebotomist or nurse to evaluate the veins
- Considering a different site if ordered by a licensed professional
- Letting the provider know if repeated attempts have failed
Clear and kind communication with the patient is just as important. A brief, honest explanation of what happened, what will happen next, and that their comfort matters helps keep trust strong.
At DuMonde Management & Consulting, we see every difficult venipuncture as a chance to grow skill and confidence. Our focus on phlebotomy training, hands-on practice, and real-world scenarios helps CNAs and other professionals turn tough veins into safer, calmer experiences for both staff and patients.
Advance Your Healthcare Career With Expert Phlebotomy Skills
If you are ready to build safer, more confident blood-draw practices, our phlebotomy training can help you move forward with clarity and purpose. At DuMonde Management & Consulting, we focus on practical, real-world skills that improve both patient safety and workflow efficiency. Let us know your goals, and we will recommend the best path to support your team or your individual career. To discuss next steps or schedule a session, please contact us today.